Introduction
Acne vulgaris is one of the most common dermatological conditions worldwide, affecting approximately 85% of adolescents and a significant number of adults. Characterized by comedones, papules, pustules, nodules, and sometimes scarring, acne can impact not only the skin but also self-esteem and quality of life. This blog post explores the different types of acne vulgaris, its underlying causes, mechanisms, treatment strategies, and essential skincare practices.
Types of Acne Vulgaris
Understanding the various types of acne is crucial for accurate diagnosis and treatment. The condition is generally categorized as:
- Comedonal Acne
- Features: Whiteheads and blackheads
- Caused by clogged hair follicles with sebum and dead skin cells
- Inflammatory Acne
- Features: Red papules and pustules
- Triggered by bacterial activity and immune response
- Nodulocystic Acne
- Features: Painful, deep nodules and cysts
- Often results in scarring and requires systemic treatment
- Acne Conglobata
- Severe, chronic form of nodulocystic acne
- Can involve multiple interconnected lesions and sinus tracts
Causes of Acne Vulgaris
Acne is multifactorial in origin. Common contributing factors include:
- Hormonal Fluctuations: Androgens increase sebum production, especially during puberty, menstruation, and stress.
- Genetic Predisposition: Family history plays a strong role.
- Bacterial Proliferation: Cutibacterium acnes (formerly Propionibacterium acnes) thrives in clogged follicles.
- Excess Sebum Production: Overactive sebaceous glands are a hallmark of acne.
- Follicular Hyperkeratinization: Increased skin cell turnover leads to clogged pores.
- Environmental Triggers: Humidity, diet, cosmetics, and stress can exacerbate symptoms.
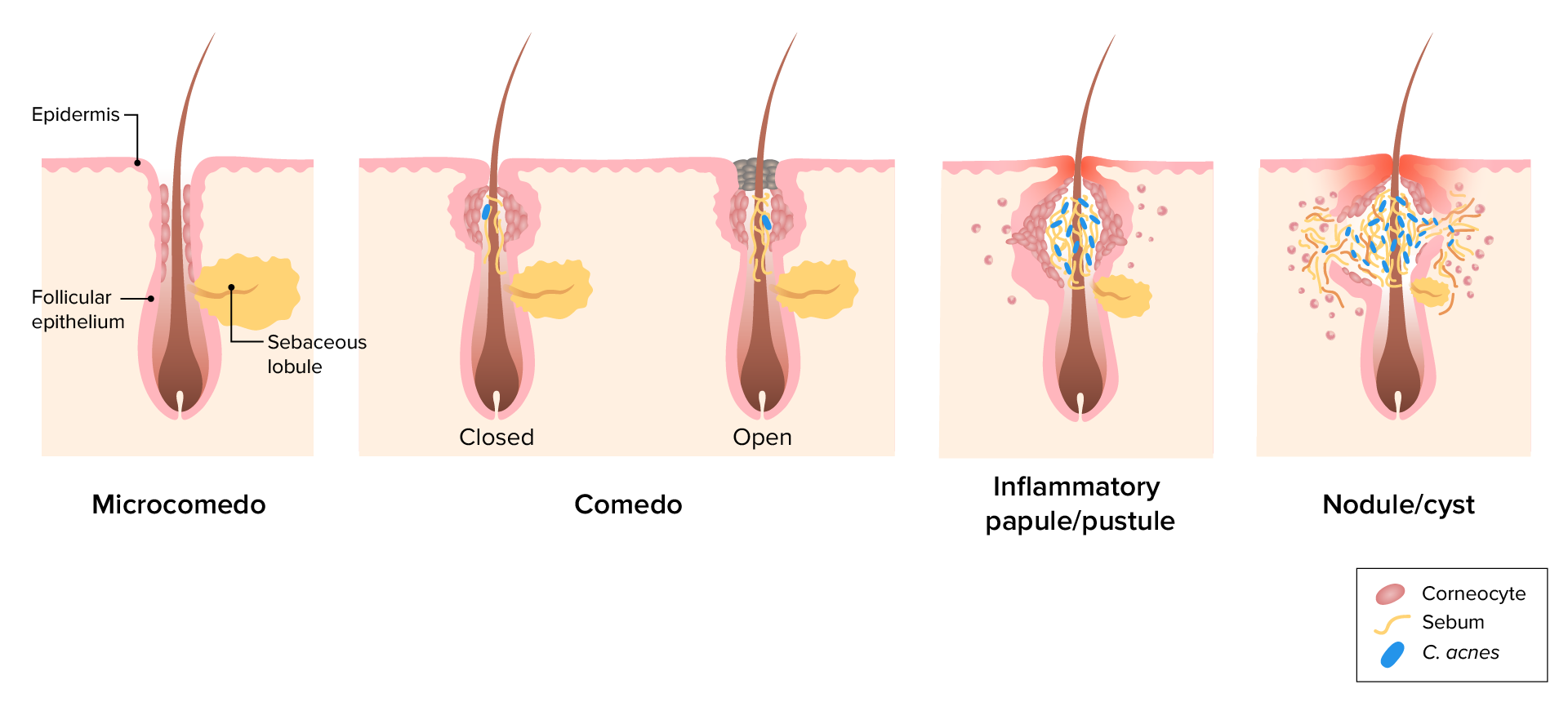
Pathophysiology: How Acne Develops
Acne vulgaris develops through a combination of four key mechanisms:
- Sebaceous gland hyperactivity under androgen influence
- Abnormal keratinization leading to comedone formation
- Bacterial colonization with C. acnes
- Inflammatory response from the immune system
These processes create a cycle of clogged pores, bacterial growth, and inflammation, which results in the various acne lesions seen clinically.

Treatment Options for Acne Vulgaris
Effective management depends on the severity and type of acne:
Topical Treatments
- Retinoids: Tretinoin, adapalene — normalize keratinization
- Antibiotics: Clindamycin, erythromycin — reduce inflammation and bacteria
- Benzoyl Peroxide: Bactericidal and keratolytic
- Azelaic Acid: Anti-inflammatory and comedolytic
Systemic Treatments
- Oral Antibiotics: Doxycycline, minocycline — used for moderate to severe inflammatory acne
- Hormonal Therapy: Combined oral contraceptives, spironolactone
- Oral Isotretinoin: Reserved for severe nodulocystic acne; targets all four pathogenic mechanisms

Procedural Therapies
- Chemical Peels
- Photodynamic Therapy (PDT)
- Laser and Light Therapy
- Comedone Extraction
Skincare Tips for Acne-Prone Skin
Maintaining an appropriate skincare routine can support medical treatment and prevent future breakouts:
- Cleanse Gently: Use a non-comedogenic, sulfate-free cleanser twice daily.
- Moisturize: Choose lightweight, oil-free moisturizers to maintain skin barrier function.
- Sun Protection: Daily use of non-comedogenic sunscreen prevents hyperpigmentation and irritation.
- Avoid Harsh Scrubs: Mechanical exfoliation can worsen inflammation.
- Non-comedogenic Products: Opt for makeup and skincare labeled “non-comedogenic.”
Conclusion
Acne vulgaris is a complex but treatable condition. Early diagnosis and a combination of medical therapy with consistent skincare can lead to significant improvements in both appearance and self-confidence. For personalized acne management, consult a board-certified dermatologist.

